By admin | Oct 07, 2016

What is Age-Related Macular Degeneration (AMD)?
Age-Related Macular Degeneration (AMD) is a degenerative eye disease affecting the macula. The macula is the part of the retina which is responsible for detailed work such as reading, driving, and recognizing people’s faces. AMD is a common condition and is one of the leading causes for loss of vision for people over the age of 50. As the severity of AMD progresses, it can significantly impact central vision, making it difficult to do detail oriented tasks such as reading and driving.
AMD Risk Factors
There are several risk factors for AMD, age being the most dominant. AMD is more likely to occur in patients over the age of 60, but can present earlier in certain cases. Other risk factors include:
Patients may be able to reduce their risk of developing AMD by not smoking, exercising regularly and maintaining healthy cholesterol and blood pressure levels, and eating lots of leafy greens and healthy fats.
What are the symptoms, types and stages of AMD?
Symptoms
Symptoms of AMD will vary slightly in type and severity from patient to patient, but most commonly straight lines gradually appear to be missing, wavy or crooked. Other symptoms might include blurriness, darkening of vision (ie. You need more light to read), difficulty recognizing faces, blind spots in central vision.
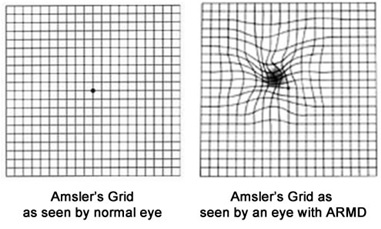

Vision with Macular Degeneration
Types
There are two different types of AMD- wet and dry, with dry AMD being the most common and only 10-20% of patients having wet AMD.
i. Dry Macular Degeneration presents with an increasing number of yellow deposits under the retina called drusen. The increasing number of drusen damages or destroy cells in the macula- subsequently affecting the vision. Dry AMD can develop into wet AMD in some cases.
ii. Wet Macular Degeneration occurs due to abnormal blood vessels growing under the macula. These new blood vessels are prone to leaking blood and fluids, causing damage to the light sensitive cells in the macula. The result is sudden decrease or loss of central vision.
Stages
i.Early AMD is diagnosed by a thorough clinical exam with a retina specialist or ophthalmologist and usually is indicated by presence of drusen. Vision loss is not always present at this point.
ii.Intermediate AMD indicated by drusen, pigment changes in the retina, or both. These changes will be determined during an exam. Patients may be experiencing some vision loss at this point, but can still remain asymptomatic.
iii. Late AMD presents with drusen, vision loss due to damage to the macula
a. Geographic atrophy – the gradual breakdown of light sensitive cells and supporting tissue in the macula cause irreversible central vision loss.
iv. Wet (Neovascular) Macular Degeneration (aka wet AMD)- abnormal growth of blood vessels which are “leaky”, leak fluid and blood causing swelling and damage to the macula. The damage is rapid and often severe.
How do I find out if I have AMD?
Early stages of AMD can be largely asymptomatic, so a regular eye exam is critical for patients over the age of 50 or who are at high genetic risk for AMD. Only a comprehensive dilated eye exam performed by your retina specialist or ophthalmologist can determine if you do in fact have AMD. This exam might include:
Your retina specialist or ophthalmologist will look carefully for drusen (yellow deposits beneath the retina- soft drusen can be indicative of AMD), leaking blood vessels, or changes in the pigmentation of the retina caused by cellular breakdown during AMD disease progression.
I have been diagnosed with Age-related Macular Degeneration- What now?
Treatment options for AMD will vary based on individual case details (ie. Type, stage, progression, etc). There is no treatment for early AMD, but leading a heart-healthy lifestyle with exercise, good diet, and use of multivitamins has been shown to be beneficial. It is highly recommended for people who are at risk for AMD to receive a comprehensive, dilated eye exam with a retina specialist or ophthalmologist at least once a year. This increases your chances of catching any disease indicators early, and you can therefore work with your retina specialist or ophthalmologist on developing a course of action, if necessary.
In the interest of maintaining further transparency and providing a wide breadth of information to our patients and providers, this blog will serve as an educational and informative resource on interesting happenings within Retina Consultants of Boston and in the greater field of Ophthalmology.
Here at Retina Consultants of Boston, Dr. John J. Weiter and Dr. Namrata Nandakumar are on the forefront of diagnostic techniques, treatment and micro-surgical techniques for macular degeneration, diabetic retinopathy, retinal detachments, macular holes, and a number of other issues affecting the vitreous and retina. Check back here frequently for news and updates on our practice and all things retina!