By admin | Aug 03, 2016

What is a posterior vitreous detachment (PVD)?
Your eye is filled with a gel-like substance called the vitreous. The vitreous helps the eye to keep its spherical shape and acts as a shock absorber in the event of trauma. The vitreous also encourages the transmission of light from the entrance in the cornea to the retina which allows you to see.
The vitreous is made of multiple components including water, collagen, proteins and hyaluronic acid. It forms a complex matrix which adheres to the back (or posterior) wall of the eye. As we age, these fibers can become crosslinked and tangled, producing traction, causing the vitreous to separate from the back wall of the eye.
PVD Symptoms and Treatment
Symptoms of a posterior vitreous detachment (PVD) include flashes and floaters. These can occur often or intermittently. Floaters usually appear suddenly and can vary in number from patient to patient. Some patients experience flashes of light, which is the tugging of vitreous gel on the retina.
Some patients experience none or all of these symptoms with varying degrees of severity. If you or someone you know experiences floaters or flashes, it is best they see their retina specialist immediately for evaluation.
The primary treatment for PVD includes close monitoring by your retina specialist. It takes several weeks for the process of a PVD occurring to completely finish. During this time frame, it is important to monitor for a retinal tear, which could lead to a retinal detachment (see below). In over 90% of the cases, a PVD occurs without any complications.
Sometimes, a PVD can result in dense floaters that do not improve over time and which impede day to day activities, such as driving. In this case, PVD could be treated using a surgical intervention called a vitrectomy. The procedure involves removing vitreous from the eye. This is an intervention which must first be deemed necessary by your retina specialist. However, most cases need little more than close monitoring through office visits with your retina specialist.
What is a retinal detachment?
The retina is a thin layer of neural tissue lining the posterior wall of the eye, not unlike wallpaper on a wall. The retina is a critical aspect of vision in that it allows light perception and converts light rays to nerve impulses which can be relayed to, and interpreted by, the brain. If the retina is damaged, vision can be severely affected.
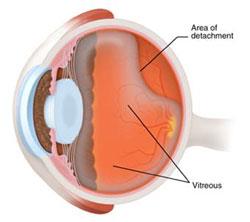
When the retina ceases to be adhered to the posterior wall of the eye, this is classified as a retinal detachment. There are 3 different types of retina detachments:
1. Rhegmatogenous- a tear in the retina where fluid accumulates underneath, separating it from the delicate epithelium underneath (this type of detachment is the most common).
2. Tractional- scar tissue on the surface of the retina produces traction and results in a detachment.
3. Exudative- most common in cases of trauma or diseases of the retina, where fluid leaks underneath the retina, but there are no tears or breaks.
What are retinal detachment causes?
In some PVD cases, the tugging of the vitreous creates enough traction to lift the retina away from the back of the eye. This can cause a tear which allows fluid to accumulate underneath the retina and separates it from its normal position; thereby causing a retinal detachment.
Alternatively, trauma can cause detachments or tears in the retina as well.
How are retina detachments treated?
There are a few different ways by which your retina specialist can opt to treat a retinal detachment. These treatment modalities will be determined by the type of retinal tear or detachment and the severity. Your retina specialist can utilize laser surgery to adhere the retina back to the wall of the eye. This is an office procedure. If the retinal detachment is severe enough, it may need to be repaired in the operating room. Your retina specialist will review all your treatment options and review why a particular option is the best fit for you. Timely repair of a retinal detachment is very important. If not repaired, it can lead to irreversible loss in vision.
As always, if you experience any changes in your vision or have questions about symptoms you may have, our retina specialists are always available for consults. Treatment approaches and outcomes vary from patient to patient, so be sure to discuss any specific details of your case with one of our physicians. As always, your vision is our greatest priority!
In the interest of maintaining further transparency and providing a wide breadth of information to our patients and providers, this blog will serve as an educational and informative resource on interesting happenings within Retina Consultants of Boston and in the greater field of Ophthalmology.
Here at Retina Consultants of Boston, Dr. John J. Weiter and Dr. Namrata Nandakumar are on the forefront of diagnostic techniques, treatment and micro-surgical techniques for macular degeneration, diabetic retinopathy, retinal detachments, macular holes, and a number of other issues affecting the vitreous and retina. Check back here frequently for news and updates on our practice and all things retina!